We all know that stones in the gallbladder or bile ducts are a cause of right upper quadrant (RUQ) abdominal pain. But did you know that there is another, just as common, cause of pain in that area that ultrasound can easily detect?
Yup, I’m talking about Adenomyomatosis of the gallbladder.
How much do you really know about this disease? Improve your knowledge and scanning skills by reading more.
Yup, I’m talking about Adenomyomatosis of the gallbladder.
How much do you really know about this disease? Improve your knowledge and scanning skills by reading more.
Histologically speaking, adenomyomatosis it causes proliferation of the mucosa of the gallbladder wall, which forms invaginations and diverticula that penetrate into the thickened muscular layer, which are know as the Rokitansky-Aschoff sinuses. These thickened areas contain small bile-filled cystic spaces, and that bile may undergo a concentration process leading to crystal precipitation and calcification. Generally speaking it is a benign hypertrophic and degenerative disease.
Adenomyomatosis is frequently associated with other biliary and pancreatic diseases, such as cholelithiasis, chronic cholecystitis, choledocholithiasis and pancreatitis. Because of this, it is believed that chronic inflammation of the biliary mucosa contributes to the cause of adenomyomatosis. This may also explain why it is more commonly seen after 50 years of age. Time + Inflammation = adenomyomatosis.
Adenomyomatosis is frequently associated with other biliary and pancreatic diseases, such as cholelithiasis, chronic cholecystitis, choledocholithiasis and pancreatitis. Because of this, it is believed that chronic inflammation of the biliary mucosa contributes to the cause of adenomyomatosis. This may also explain why it is more commonly seen after 50 years of age. Time + Inflammation = adenomyomatosis.
So, why is it important to find Adenomyomatosis?
Getting a requistion for RUQ pain is pretty common, and we sonographers don’t always find the cause of that patient’s pain, which can feel pretty frustrating. But once you are aware that adenomyomatosis can also be a cause of pain, you may find that you see it more often than you think. Adenomoyomatosis occurs almost as frequently (9%) as gallstones do (10%) in the general population, so it’s worth remembering to carefully assess the gallbladder area for it.
Adenomyomatosis can also cause significant abdominal pain, RUQ pain and hepatic colic, but it can also be asymptomatic. It occurs in both the presence and absence of gallstones. However, it is important to note that adenomyomatosis is a distinct pathology seperate from cholelithiasis and cholecystitis.
Once identified, symptomatic adenomyomatosis is an indication for cholecystectomy, which results in complete disappearance of symptoms in upwards of 90% of patients. Some forms of adenomyomatosis can also be associated with galllbladder carcinoma or leiomyosarcoma, especially in elderly patients.
Which brings up the important question of...
Adenomyomatosis can also cause significant abdominal pain, RUQ pain and hepatic colic, but it can also be asymptomatic. It occurs in both the presence and absence of gallstones. However, it is important to note that adenomyomatosis is a distinct pathology seperate from cholelithiasis and cholecystitis.
Once identified, symptomatic adenomyomatosis is an indication for cholecystectomy, which results in complete disappearance of symptoms in upwards of 90% of patients. Some forms of adenomyomatosis can also be associated with galllbladder carcinoma or leiomyosarcoma, especially in elderly patients.
Which brings up the important question of...
How to find Adenomyomatosis with ultrasound?
Adenomyomatosis, whether symptomatic or not, will show up on ultrasound as an enlarged gallbladder wall, greater than 3 mm in thickness (in a non-contracted gallbladder, or after patient has fasted for a minimum of 8 hrs).
This thickened gallbladder wall is most commonly seen in the fundas, but can also occur in the neck area, as well as mid body in a ring-like shape, or generalized over a large area.
This thickened gallbladder wall is most commonly seen in the fundas, but can also occur in the neck area, as well as mid body in a ring-like shape, or generalized over a large area.
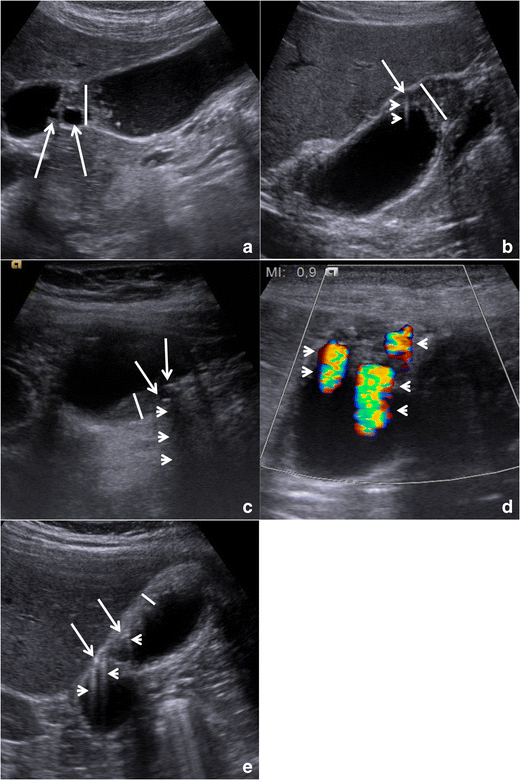
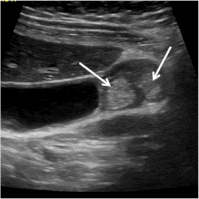
Gallbladder adenomyomatosis: typical ultrasound findings. Wall thickening (line) is always seen in gallbladder adenomyomatosis, but it can be non-specific. On b-mode images, Rokitansky–Aschoff sinuses (RAS) (arrows) typically appear anechoic (a), but they can also appear hyperechoic if crystals or calcifications are present (b and c). Comet-tail reverberation artefacts (Figures b and e, arrowheads) or acoustic shadowing (c, arrowheads) are usually observed in RAS. On colour Doppler images (d), twinkling artefacts (arrowheads) may be observed in RAS.
Recommended TIPS for Assessment OF gallbladder FOR adenomyomatosis
1. Precise focal depth adjustment is necessary when assessing the gallbladder wall, as often a more superficial focal point is needed to adaquately assess the fundal area (where adenomyomatosis is most commonly found).
2. It is also advised to use a high frequency probe – since the gallbladder fundas can be quite superficial, it is unsatisfactorily evaluated with a 4-5MHz convex transducer. Suspicious findings in this area are better visualized by a higher frequency (7-9 Mhz) linear transducer (link to linear transducer article).
3. Harmonic imaging is also something that will increase the visualization of the gallbladder wall and the detection of Rokitansky-Aschoff sinuses. Use hepatic tissue as a window between the transducer and the gallbladder to also increase image quality.
4. Use multiple windows to assess the anterior wall of the gallbladder very closely for any of the following: thickening (focal or diffuse), areas of irregularity, small cysts and also tiny hyperechoic points (where the bile has crystallized or calcified and creates shadowing), 2D comet tail artifact, color doppler artifact of twinkling, or both.
5. It’s also important to assess any areas of thickened gallbladder wall with color or power doppler, the presence of Rokitansky-Aschoff sinuses will appear avascular, so the presence of any vascularity within a thickened wall should be suspicious for malignancy.
Remember that ultrasound is an operator-dependent imaging modality and the depiction of the gallbladder will vary according to the operators (your) experience.
Take care with gallbladder assessment, remember to always optimize for the organ you are assessing, ask for a second opinion from a fellow tech when you are not sure of something, and use a cine-loop to show any complex or confusing pathology in real-time.
Happy Scanning!
Note:
Images reprinted from the SpringerLink article Gallbladder adenomyomatosis: imaging findings, tricks and pitfalls,(https://link.springer.com/article/10.1007%2Fs13244-017-0544-7) under the terms of the Creative Commons CC BY license.
References and more information:
Gallbladder adenomyomatosis: imaging findings, tricks and pitfalls
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5359147/#!po=28.7234
https://link.springer.com/article/10.1007%2Fs13244-017-0544-7
Gallbladder adenomyomatosis: Diagnosis and management
https://www.ncbi.nlm.nih.gov/pubmed/28844704
Adenomyomatosis of the gallbladder
https://www.ncbi.nlm.nih.gov/pubmed/1154265
Diffuse Adenomyomatosis Of The Gallbladder: An Infrequent Disease Wth Difficult Preoperative Diagnosis
http://ispub.com/IJS/10/1/6939#
2. It is also advised to use a high frequency probe – since the gallbladder fundas can be quite superficial, it is unsatisfactorily evaluated with a 4-5MHz convex transducer. Suspicious findings in this area are better visualized by a higher frequency (7-9 Mhz) linear transducer (link to linear transducer article).
3. Harmonic imaging is also something that will increase the visualization of the gallbladder wall and the detection of Rokitansky-Aschoff sinuses. Use hepatic tissue as a window between the transducer and the gallbladder to also increase image quality.
4. Use multiple windows to assess the anterior wall of the gallbladder very closely for any of the following: thickening (focal or diffuse), areas of irregularity, small cysts and also tiny hyperechoic points (where the bile has crystallized or calcified and creates shadowing), 2D comet tail artifact, color doppler artifact of twinkling, or both.
5. It’s also important to assess any areas of thickened gallbladder wall with color or power doppler, the presence of Rokitansky-Aschoff sinuses will appear avascular, so the presence of any vascularity within a thickened wall should be suspicious for malignancy.
Remember that ultrasound is an operator-dependent imaging modality and the depiction of the gallbladder will vary according to the operators (your) experience.
Take care with gallbladder assessment, remember to always optimize for the organ you are assessing, ask for a second opinion from a fellow tech when you are not sure of something, and use a cine-loop to show any complex or confusing pathology in real-time.
Happy Scanning!
Note:
Images reprinted from the SpringerLink article Gallbladder adenomyomatosis: imaging findings, tricks and pitfalls,(https://link.springer.com/article/10.1007%2Fs13244-017-0544-7) under the terms of the Creative Commons CC BY license.
References and more information:
Gallbladder adenomyomatosis: imaging findings, tricks and pitfalls
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5359147/#!po=28.7234
https://link.springer.com/article/10.1007%2Fs13244-017-0544-7
Gallbladder adenomyomatosis: Diagnosis and management
https://www.ncbi.nlm.nih.gov/pubmed/28844704
Adenomyomatosis of the gallbladder
https://www.ncbi.nlm.nih.gov/pubmed/1154265
Diffuse Adenomyomatosis Of The Gallbladder: An Infrequent Disease Wth Difficult Preoperative Diagnosis
http://ispub.com/IJS/10/1/6939#